Infusion centers are under incredible pressure to treat more patients with fewer resources. iQueue for Infusion Centers unlocks capacity to safely increase patient access to life-saving services.
800+
Infusion Centers
16k
Infusion Chairs
$20k
Infusion Chair/Year in ROI
720k
Additional Treatments/Year
Infusion centers struggle with unique operational challenges, like managing patient appointments linked to clinics, labs, and pharmacies, retaining specialized nurses, and rising patient demand. This often leads to volatile workloads in which resources may be both under- and over-utilized in the course of a single day, every day. Traditional methods like grid-based scheduling and first-call-first-scheduled don’t work. Plus, there are incredible intricacies to scheduling linked appointments that manual processes can’t address.
iQueue for Infusion Centers leverages machine learning and predictive analytics to help centers stay operationally agile by optimizing their scheduling templates, level-loading the daily schedule across the nursing staff, flagging future problem days for preventive action, and identifying which appointments should be rescheduled to improve the experience for patients and staff alike.

Manage the day before it unfolds or look 4 weeks ahead with huddle reports that include expected chair utilization, template compliance, and over/under-booking estimations to manage unforeseen bottlenecks, add-ons, and no shows.
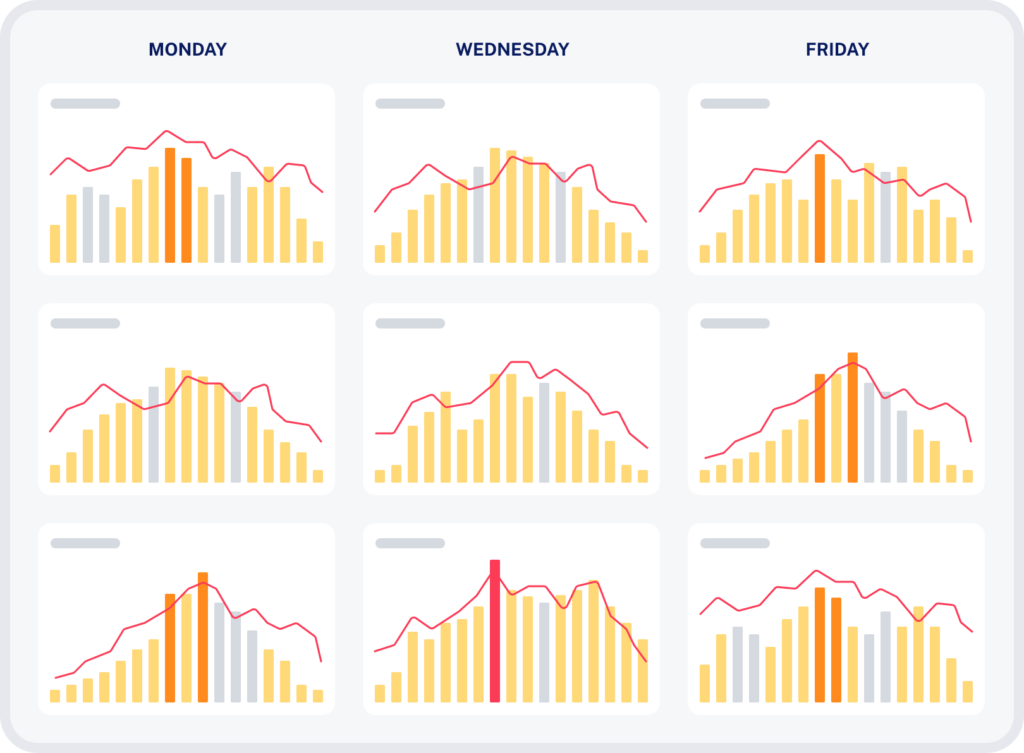
Optimize scheduling with custom templates based on your historical data and unique infusion center goals to maximize patient access, accommodate linked appointments, decrease wait times, and level load the day.
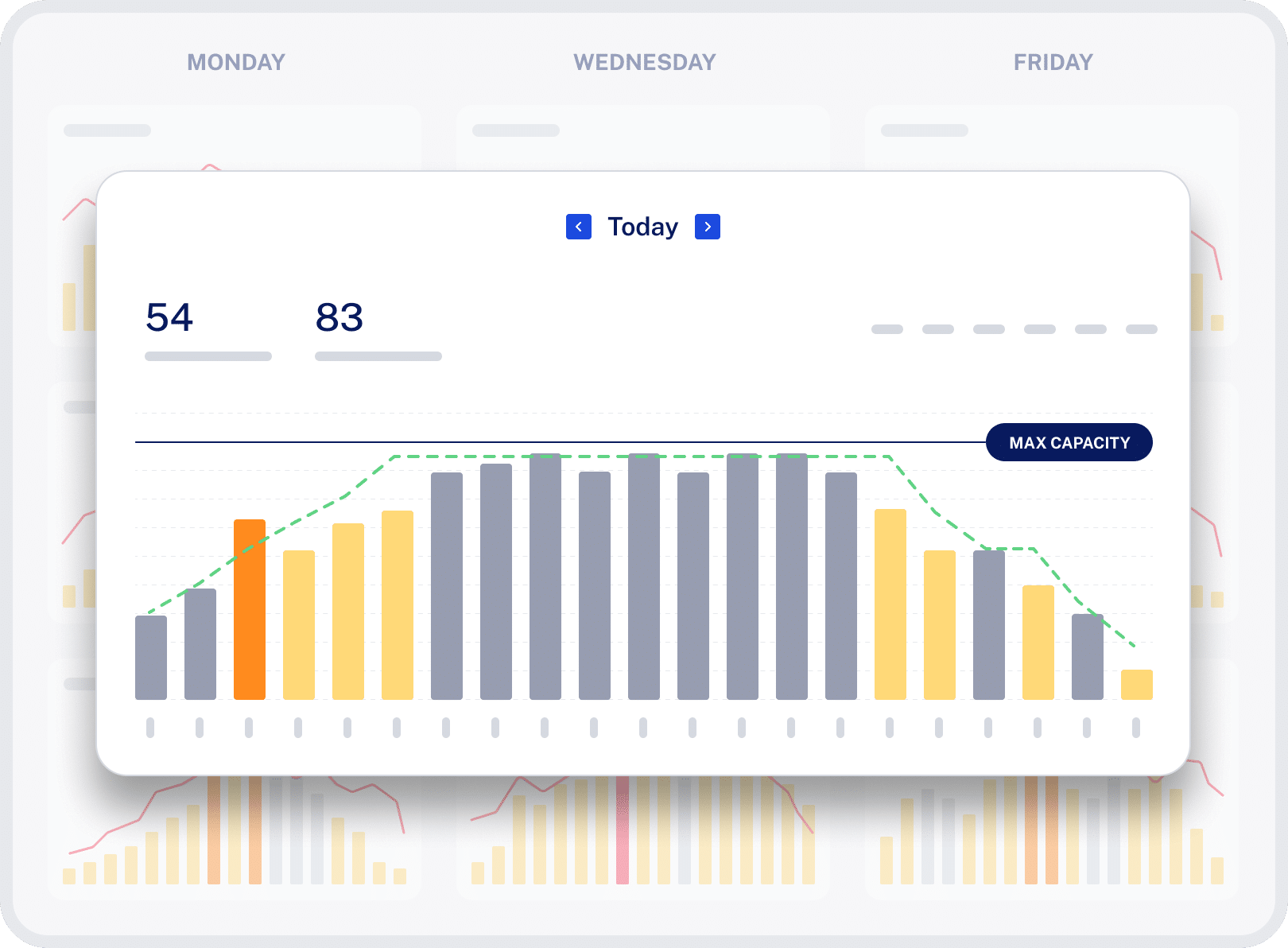
Manage and predict appointments and staffing needs with real-time insights to avoid the “midday chaos”, missed lunches, and excessive overtime that leads to burnout and dissatisfaction.

Improve capacity management and eliminate manual administrative tasks with automated, intelligent reports that help staff monitor performance goals, make proactive decisions, and quickly spot operational issues that need attention.
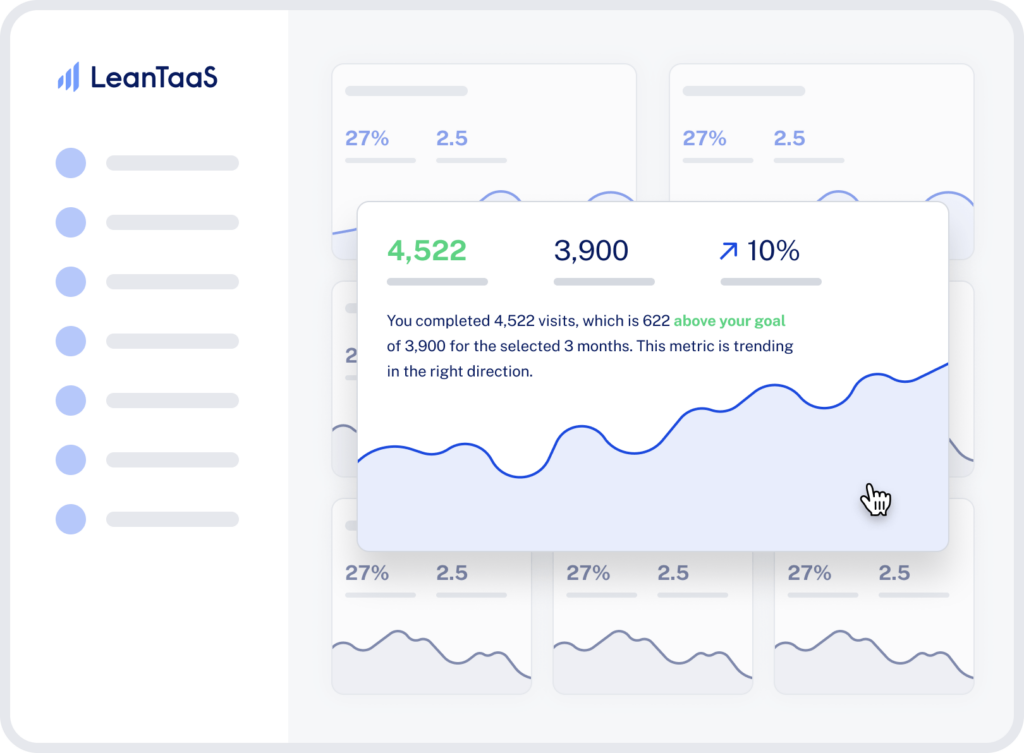

With the implementation of iQueue, we were able to increase our volumes by 18%, decrease our wait times for access to a chair by 44%, and lower the wait time for drugs from the pharmacy by 25% due to decreasing the morning bottlenecks we were experiencing.
We weren’t using our resources effectively, and our most valuable resource is [people]. After adopting iQueue, the number of days when infusion centers operated past their scheduled closing times decreased by 31%. Nurses could actually rely on being finished at 5:30 p.m., which improved their ability to make plans after the workday.
It’s quite miraculous to me that we had this increase in patient volume at a time when we were having to go through all of the COVID restrictions.




Take the first step towards unlocking capacity, generating ROI, and increasing patient access.
When we started with iQueue we had an average daily volume of 98 appointments a day and we now have 117 appointments per day. So that’s about an average of 19 new patients, new appointments that we are seeing each day or 95 additional appointments throughout the week…essentially we have added an entire day of treatment to our week.